 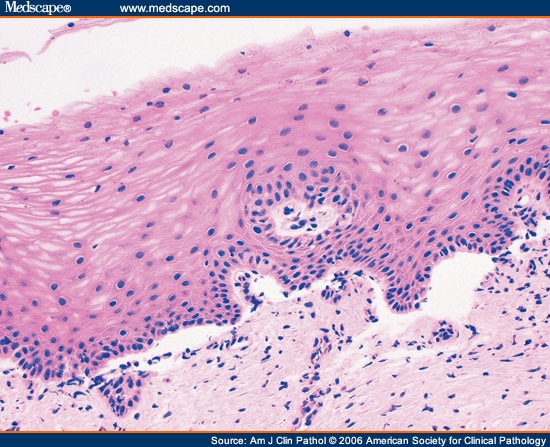
24 Low levels of fusion transcript were not observed in two other studies of normal endometrium. 23 In one study, low levels of JAZF1-JJAZ1 fusion transcript messenger RNA, as well as its protein product, were detected in normal endometrial stromal cell lines and in normal late secretory endometrial tissues. 22 Several other fusion transcripts have been identified in ESTs, including transcripts involving the PHD finger protein 1 (PHF1), enhancer of polycomb 1 (EPC1), and 14-3-3 genes. 
7, 11, 17–21 A subsequent study examining the frequency of gene rearrangements in 94 ESTs found that the JAZF1-JJAZ1 fusion transcript could be detected in 50% of ESNs (4/8) and 70% of ESTs (28/40). 16 The JAZF1-JJAZ1 fusion transcript as well as the t(7 17)(p15 q21) has been detected by reverse transcriptase–polymerase chain reaction and fluorescence in situ hybridization in 76% of ESNs (16/21), 58% of ESSs (43/74), and 20% of UESs (2/10). 11 This fusion, between the juxtaposed with another zinc finger 1 ( JAZF1) and the joined to JAZF1 ( JJAZ1) genes, leads to expression of a fusion protein that, in cultured human embryonic kidney 293 cells, leads to resistance to apoptosis and, when the unrearranged JJAZ1 protein is suppressed, increased rates of proliferation. 7 The characteristic molecular alteration found in ESTs is the recurrent chromosomal translocation t(7 17)(p15 q21), which leads to production of JAZF1-JJAZ1 fusion RNA. 8–15 This nonrandom t(7 17) and its variants have been detected in 31% of the karyotypes reported to date, as summarized in a recent comprehensive review. 7 The most frequent chromosomal rearrangement is a translocation between the short arm of chromosome 7 and the long arm of chromosome 17. 1ĮSTs are characterized by specific chromosomal and molecular alterations. After tumor type has been established, stage of disease is the most significant prognostic factor. Correct diagnosis is, however, of great clinical importance. 1 The diagnosis of EST on uterine biopsy can be extremely challenging due to its resemblance to proliferative endometrial stroma. 6 One-third to half of ESSs present with spread outside the uterus. The most frequent presenting symptom for both ESNs and ESSs is vaginal bleeding. 4, 5 UES, meanwhile, is an aggressive neoplasm with extensive cell atypia and necrosis. The diagnosis of these tumors on light microscopy is complicated by the presence of a number of variant forms, including smooth muscle differentiation, glandular and epithelial differentiation, and sex-cord differentiation. 4 On biopsy material, a diagnosis of EST is often used because tumor circumscription cannot be determined. The distinction between the two rests on the evaluation of tumor circumscription, both macroscopically and microscopically. 3 Both ESN and ESS are low-grade tumors composed of a monotonous population of cells with a delicate vasculature resembling normal proliferative phase endometrial stroma. 
In the 2003 World Health Organization classification of tumors, they are divided into endometrial stromal nodule (ESN), endometrial stromal sarcoma (ESS), and undifferentiated endometrial sarcoma (UES). 1, 2 They are the second most common uterine mesenchymal tumor after leiomyosarcoma. They constitute less than 10% of all uterine malignancies and approximately 20% of all uterine sarcomas. Endometrial stromal tumors (ESTs) are rare mesenchymal tumors occurring primarily in the uterine corpus. 
0 Comments
Leave a Reply. |
AuthorWrite something about yourself. No need to be fancy, just an overview. ArchivesCategories |



 RSS Feed
RSS Feed
